Our Capabilities
Payer Market Access Services

Navigate market complexity,
empower access, elevate outcomes
One-third of U.S. drug and device launches underperform due to misaligned strategy and poor execution. Payer access is one of the most intricate challenges in the pharmaceutical industry, requiring a multi-faceted strategy that aligns clinical value with payer priorities. Success depends on navigating complex systems, building compelling value propositions, and executing seamlessly across multiple phases.
At TJP, we leverage our team’s extensive payer-side experience and network to develop tailored strategies for achieving access wins—and ensuring that access translates to successful adoption and patient uptake.

A deeply embedded team with 20+ years of experience developing nimble, high-impact strategies
In an industry where payer requirements and market dynamics are constantly evolving, pharmaceutical companies deserve an agency of record that can function as a trusted partner ready to guide products from pre-launch planning to loss of exclusivity.
TJP offers personalized, agile market access support, providing clients with a dedicated team and unmatched commitment.
Experienced industry perspectives:
TJP’s Market Access Council
The TJP Market Access Council is a standing resource designed to help address the complexities of market access and achieve optimal outcomes through proactive consultations and material review.
- Expert perspectives that shape access strategies across the product life cycle
- Actionable insights to support pre-approval planning, launch execution, and postlaunch optimization
- Review of materials to align with payer expectations and evolving market dynamics
- Real-world feedback to navigate complex healthcare challenges effectively
Payer Access Council Experts
- VP of Pharmacy at one of the leading integrated healthcare systems in the nation
- Pharmacy Director at UnitedHealthcare
- CMO of a division of Humana
- Executive at MedImpact, Diplomat, and Kelsey-Seybold
- Express Scripts clinical and contracting executive
Compelling data, authoritative payer engagement
Our team focuses on the metrics that matter most to payers and thought leaders, tapping into diverse Health Economics Outcomes Research (HEOR), Real World Evidence (RWE), and real-time analytics to articulate data-rich, authoritative value propositions for client brands.
Evidence Synthesis
Systematic literature reviews (SLRs)
Meta-analyses
Pooled individual patent data (IPD)
Network meta-analyses
Indirect treatment comparisons (ITCs)
Health Economics and Strategy
Evidence strategy consulting
Evidence development and testing
Economic models
Healthcare costs and resource use
Dossier development
Regulatory support
Epidemiology, Health Outcomes, and Observational Studies
Real-world evidence analytics
Trial-based analytics
Treatment patterns and outcomes
Comparative effectiveness studies
Surveillance and natural history studies
Patient-Centered Research
Patient journey studies
Patient and caregiver burden
Survey development and implementation
Quality-of-life studies
Collaborative strategies, adaptable execution
We deliver payer access strategies built to adapt to the evolving formulary landscape, emerging competitive threats, and regulatory changes.
Our adaptive approach ensures value messaging evolves with real-world insights, transitioning from pre-launch hypotheses to post-launch evidence that resonates with payers.
Hands-on problem-solving, comprehensive support
We tackle access challenges by targeting specific barriers such as prior authorization challenges and formulary gaps. Our solutions are integrated as holistic value communications ecosystems, including everything from pull-through strategies that simplify access and enhance engagement, to the development of tailored solutions like cost calculators.
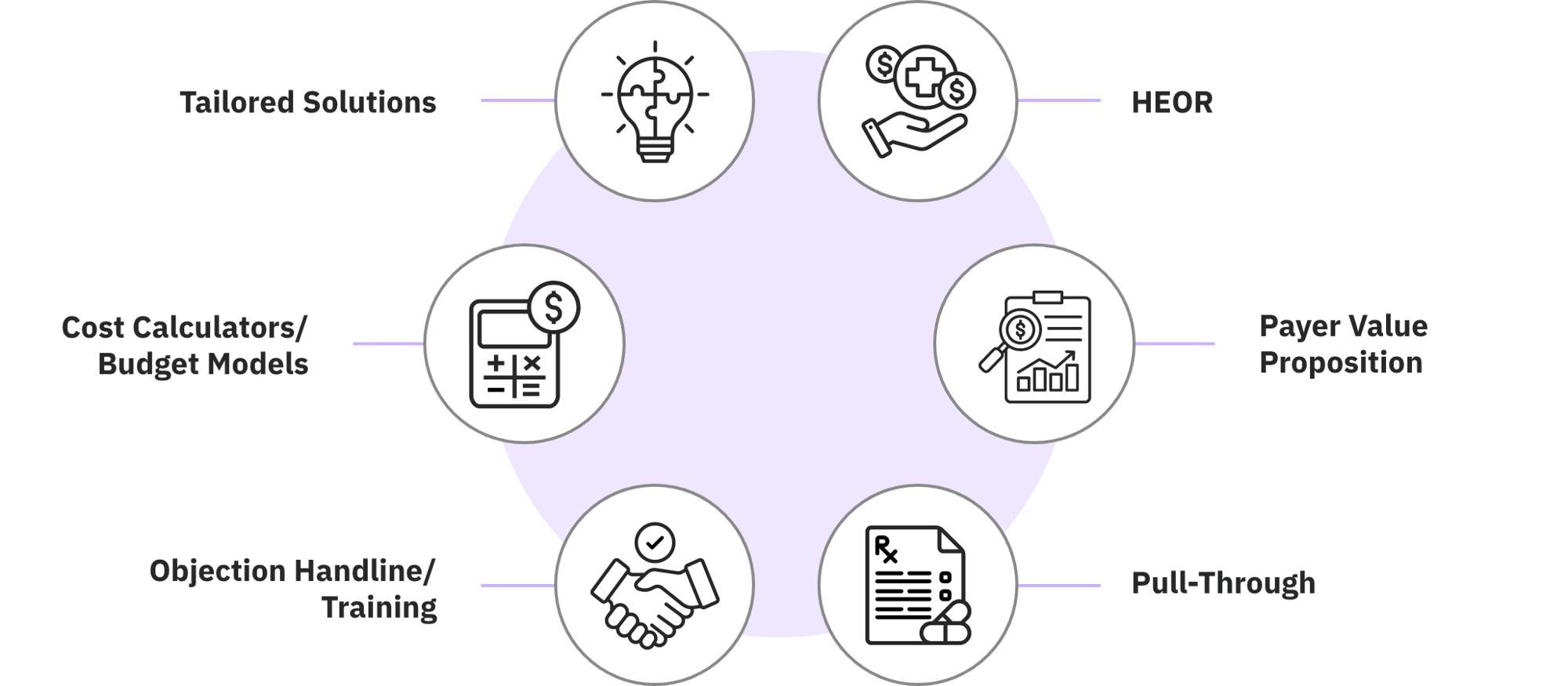
Strong payer partnerships, powerful product narratives
We have the relationships needed to quickly and effectively engage key decision-makers in major payer organizations through carefully targeted product storytelling centered on payer value. Engaging with Integrated Delivery Networks (IDNs) and Group Purchasing Organizations (GPOs) demands a customized approach that balances their distinct priorities, from reducing costs to achieving better clinical outcomes.
Research & Stakeholder Mapping
Segment Stakeholders
Provider GPOs:
Centralized purchasing, clinical differentiation, focus on compliance tools
Payer GPOs:
Formulary inclusion, rebates, cost-of-care alignment
IDNs:
Balance payer (cost) and provider (clinical, opterational) priorities focus on cost-of-care metrics (e.g., Qualys)
Strategic Messaging
Tailored Value Propositions
Administrative:
Financial savings, affordability programs
Providers/Physicians:
Patient outcomes, ease of prescribing, adherence, provider value scoring
Pharmacy Directors:
Operational fit, formulary alignment
Engagement & Outcomes
360º Approach
In-Person:
Stakeholder meetings with tailored leave-behinds
Digital Pull-Through:
Relationship management, email communications
Virtural Support:
Webinars on clinical data
RWE Outcomes:
Cost reductions, improved patient outcomes
How we execute true end-to-end payer access strategies
Discover
+Uncover critical insights through rigorous research, evidence analysis, and payer interviews to lay the foundation for a winning access strategy.
- Conduct insight mining, study design analysis, feasibility study reports, and evidence gap analysis.
- Develop competitor assessments.
- Lead in-depth interviews with payer and channel key opinion leaders.
Craft
+Analyze customer needs and challenges to develop refined, payer-tested value messages and actionable strategies.
- Complete customer, channel, and distribution analysis.
- Review care pathway, burden of illness, and unmet medical need considerations.
- Refine payer-tested value messages.
Navigate
+Develop and test value-driven messaging with key stakeholders, executing strategies that address brand priorities and market demands.
- Identify disease state and key brand performance drivers.
- Test value messaging with payer channel decision-makers.
- Optimize value messaging based on testing.
Launch
+Bring strategies to life with precise execution, driving market access success and ensuring sustained impact throughout the product lifecycle.
- Identify tactics through rigorous customer research and in-depth insights to deliver on developed strategies.
- Support pull-through and patient access initiatives to maximize demand.
- Refine strategies dynamically based on market feedback to maintain relevance and optimize outcomes.
Comprehensive pharmaceutical marketing support
TJP’s payer access services are just one piece of our holistic approach to navigating market complexities and empowering your brand’s success. From strategy development to execution, we provide tailored solutions that deliver measurable outcomes and drive meaningful impact.
Discover how our full suite of capabilities can support every stage of your product’s lifecycle:
